Why Is My Thyroid Medication Not Working Anymore? Leaky Gut and Hypothyroidism Treatment with Ayurveda

Why Is My Thyroid Medication Not Working Anymore? The Leaky Gut–Thyroid Axis, Research Gaps, and an Ayurvedic Healing Protocol
If your levothyroxine dose keeps rising but your symptoms won’t budge, the missing piece may be a leaky gut. Explore the gut-thyroid connection, research gaps, and an evidence-backed Ayurvedic healing protocol that addresses the root cause.
Here’s the short answer, the one I’d want if I were a patient staring at a bottle of pills that no longer seem to work: a “leaky gut” can silently undo everything your thyroid medication is trying to do. When the intestinal lining becomes inflamed and too permeable, two things happen. First, you stop absorbing levothyroxine properly. Second, your body struggles to convert T4 into the active T3 it actually needs. The usual culprits—SIBO, H. pylori, gluten, and stubborn dysbiosis—keep that fire smouldering. The fix isn’t another dose increase. It’s repairing the gut itself. And that often leads you, surprisingly, straight into the time-tested logic of Ayurveda.
Clinician’s Corner
Primary sources: Endocrine Practice (2024, 2025), Cureus (2022), Endocrine and Metabolic Science (2024), and Ayurvedic clinical trials.
What frustrates both patients and clinicians most is not abnormal lab work — it’s the mismatch between “normal” numbers and a body that still feels profoundly hypothyroid. Many patients take levothyroxine perfectly, follow every instruction carefully, and yet continue to struggle with brain fog, fatigue, constipation, weight gain, cold intolerance, and low energy.
The problem is increasingly pointing toward the gut.
Many patients exploring a root-cause approach eventually discover that true recovery requires a broader systems perspective—one that integrates metabolism, digestion, inflammation, stress physiology, and lifestyle restoration together. That’s precisely why modern patients are increasingly turning toward holistic Ayurvedic healing protocols that address the body as an interconnected ecosystem rather than isolated symptoms alone.
Table of Contents
The Problem – When Normal Labs Hide a Broken System The Discovery – Mapping the Gut-Thyroid Sabotage The Gaps – Where Science Hasn’t Yet Caught Up The Ayurvedic Lens – Agni, Ama, and the Gut-Thyroid Connection Phase 1 – Ignite & Cleanse Phase 2 – Seal & Shield Phase 3 – Rejuvenate & Restore Frequently Asked QuestionsThe Problem – Thyroid Medication Not Working: When Normal Labs Hide a Broken System
Ask any functional or integrative clinician what frustrates them most, and they’ll describe exactly this: a hypothyroid patient who is doing everything right. They take their pill on an empty stomach. They wait the required hour. Their TSH comes back “within range.” And yet they remain deeply symptomatic. Brain fog stubbornly refuses to lift. Weight clings on. Hands stay cold. Exhaustion sits in the bones.
The standard move is to increase the levothyroxine dose. And for many, that works—until it doesn’t. A growing pile of clinical evidence now points to something far more common than we used to admit: a hefty chunk of patients labelled “refractory” aren’t non-compliant. They’re non-absorbers. And the seat of that malabsorption is almost always the small intestine.
This gut-centered perspective also aligns closely with traditional Ayurvedic frameworks that examine how impaired digestion, sluggish metabolism, and inflammatory accumulation interact together over time. If you want a broader understanding of how Ayurveda interprets chronic health dysfunction, this Ayurveda guide to chronic health issues offers deeper foundational context.
Levothyroxine is fussy. Under ideal conditions, about 62–82% of an oral dose gets absorbed in the jejunum and upper ileum. That process demands an intact gut lining, enough stomach acid, and a reasonably balanced microbial community.
But when the gut becomes inflamed and hyperpermeable—what we commonly call leaky gut—all three conditions fall apart.
Worse, the damage doesn’t stop at absorption. A leaky gut is also an immune-inflammatory bonfire that directly interferes with T4-to-T3 conversion. The result? Deceptively normal blood work alongside profoundly hypothyroid cells. That’s the hidden crisis in thyroid care.
Why “Normal Labs” Can Still Mean You Feel Terrible
- TSH may normalize even while cellular thyroid signalling remains impaired.
- Inflammatory cytokines can blunt thyroid receptor sensitivity.
- Poor gut integrity interferes with nutrient absorption required for hormone conversion.
- Microbial imbalance disrupts enterohepatic recycling of thyroid hormones.
- Stress hormones and systemic inflammation further suppress T4-to-T3 conversion.
In other words, many patients aren’t failing thyroid medication. Their gastrointestinal environment is failing the medication first.
The Discovery: Mapping the Gut-Thyroid Sabotage (Leaky Gut and Hypothyroidism Treatment)
To pull a non-responding patient out of limbo, we first have to figure out exactly what’s sabotaging their thyroid replacement. The diagnostic path I outline here blends solid gastroenterology with a functional medicine lens—and it starts with a test that is criminally underused.
1. The Levothyroxine Absorption Test – Your First Gold Standard
Before ordering a dozen expensive labs, I’ve learned to ask a simpler question first: is this patient actually absorbing their levothyroxine?
Enter the absorption test—a supervised morning dose followed by TSH and free T4 checks over the next four to six hours.
A 2025 Endocrine Practice paper confirmed what many functional clinicians already knew: a flat line on that test tells you the problem is real and it’s in the gut.
It’s one of the most overlooked tools we have. I’ve seen it turn a desperate, multi-year case of “unexplained” hypothyroidism into a straightforward gut protocol by lunchtime.
2. Biomarkers That Actually Tell You Something
Moving beyond TSH and free T4, when a patient tells me their thyroid medication stopped working, I immediately add:
Zonulin
This is the gatekeeper protein that regulates intestinal tight junctions. A 2025 cross-sectional study found that zonulin levels above 17 ng/ml predicted TPO antibody positivity with 71.67% sensitivity and a staggering 100% specificity.
If zonulin is elevated, you’ve got objective evidence of a leaky gut, and you’ve got a clear target.
Emerging research around intestinal permeability and autoimmune activation continues to strengthen the scientific basis for the gut-thyroid connection. Research published through the National Center for Biotechnology Information has increasingly explored how gut barrier dysfunction influences systemic inflammatory disease patterns.
Diamine Oxidase (DAO)
Leaky gut frequently drives histamine intolerance, causing palpitations, hives, flushing, and brain fog—symptoms that masquerade beautifully as poorly controlled hypothyroidism.
Low DAO activity unmasks this mimic.
Lipopolysaccharides (LPS)
When the gut barrier fails, endotoxins from gram-negative bacteria slip into the bloodstream.
Elevated LPS is a direct measure of metabolic endotoxemia—systemic inflammation that blunts thyroid receptor sensitivity and pours fuel on autoimmunity.
3. The Gut Map: Finding the Chief Culprit
Leaky gut rarely exists alone. Behind almost every case of levothyroxine malabsorption gut healing, there’s a primary driver. Here are the big ones I see again and again.
a) Small Intestinal Bacterial Overgrowth (SIBO)
A 2024 Endocrine Practice study found that 65.3% of hypothyroid patients with IBS-type symptoms tested positive for SIBO. And because hypothyroidism slows the gut to a crawl, it hands SIBO a perfect breeding ground.
This slowed metabolic environment is one reason many patients simultaneously experience symptoms associated with a chronically slow metabolism , including fatigue, weight resistance, poor digestion, and persistent bloating.
The overgrowth competes for nutrients, damages the brush border, and literally consumes thyroxine before it can be absorbed.
In that same study, when patients were switched from tablet to liquid levothyroxine—a formulation that bypasses much of the digestive gauntlet—77.55% normalized their TSH without any dose increase.
A simple formulation change can be profoundly revealing.
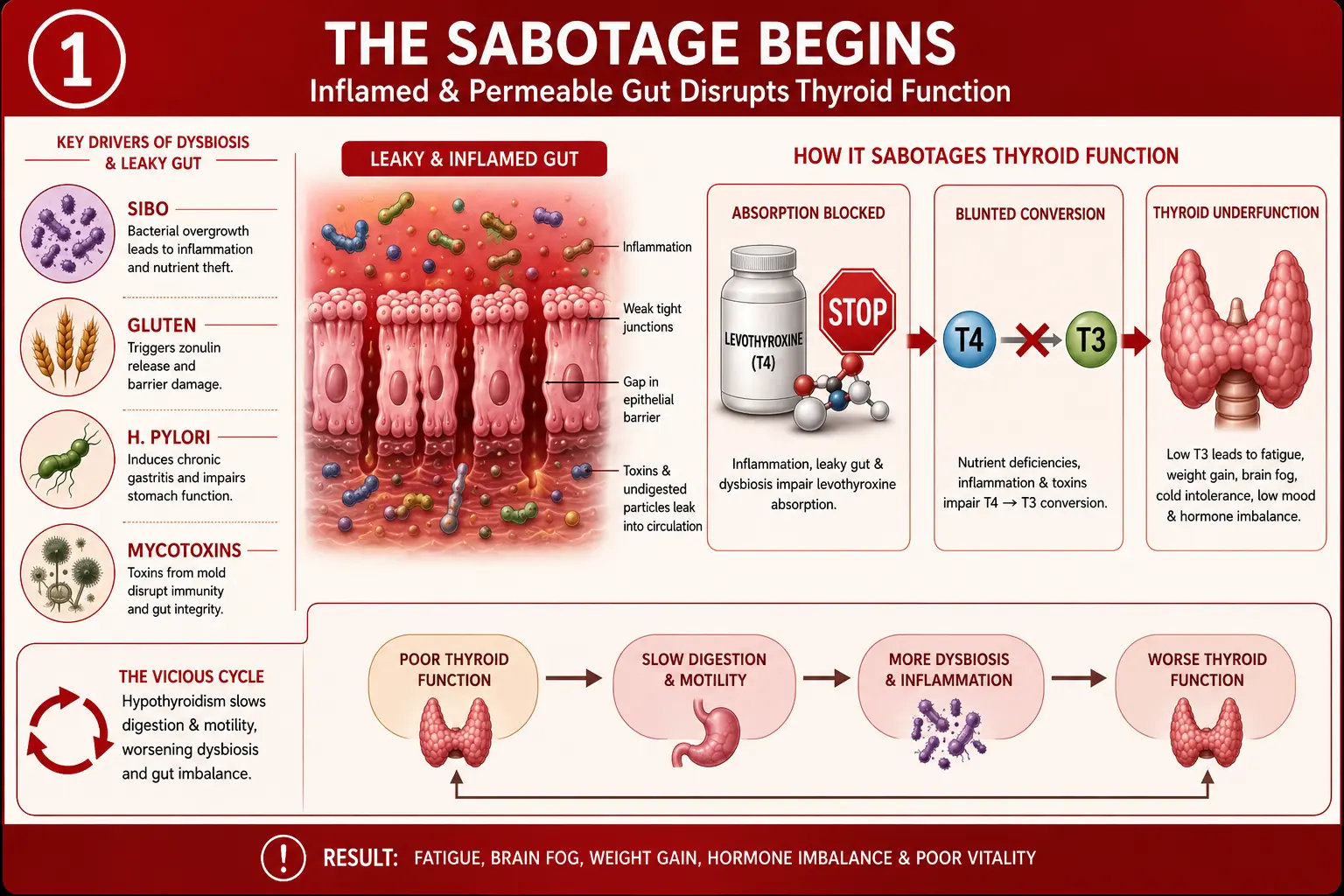
b) H. pylori Infection
This bug is a master saboteur. It induces gastric atrophy, raises stomach pH, and messes with levothyroxine dissolution.
More insidious still, molecular mimicry between H. pylori antigens and thyroid tissue can trigger autoimmunity.
Why H. pylori Matters So Much
- Raises stomach pH and impairs levothyroxine breakdown
- Weakens nutrient absorption
- Promotes chronic gastric inflammation
- Can worsen Hashimoto’s autoimmunity
- May force progressively higher medication doses
A 2022 case report in Cureus described a patient requiring supratherapeutic doses; after H. pylori eradication, thyroid requirements normalized completely.
If a patient’s dose keeps creeping up without explanation, testing for H. pylori isn’t optional—it’s essential.
c) Celiac Disease & Non-Celiac Gluten Sensitivity
The link is now ironclad. Gluten-driven inflammation flattens the very villi where levothyroxine is absorbed.
Stress physiology also plays a surprisingly powerful role here. Chronic nervous system activation alters gut permeability, stomach acid production, microbial balance, and motility simultaneously. In many patients, unresolved emotional stress becomes one of the invisible accelerants behind persistent digestive dysfunction and thyroid instability. This deeper gut-brain connection is explored further in this guide on how stress contributes to chronic stomach issues .
Multiple studies confirm that a strict gluten-free diet, especially when paired with an oral LT4 solution, resolves malabsorption and often permits dose reduction.
Even without full-blown celiac antibodies, low-grade gluten-induced enteropathy can keep the gut just irritated enough to block hormone uptake.
d) Mycotoxin Exposure
This one doesn’t get nearly enough airtime.
Mycotoxins from water-damaged buildings do two things: they loosen tight junction proteins, and they depress deiodinase type 1 activity in the liver and gut—blocking T4-to-T3 conversion.
Together, that’s a gut-thyroid wrecking ball.
Environmental Clues Often Missed
- History of living in water-damaged buildings
- Musty smell exposure
- Symptoms worsening indoors
- Unexplained fatigue alongside sinus or respiratory irritation
- Persistent inflammation despite “clean” diets
A detailed environmental history belongs in every refractory thyroid workup.
The Gaps: Where Science Hasn’t Yet Caught Up
A genuinely authoritative article needs to be honest about what we don’t yet know. These four gaps are the frontier—and they also explain why an integrative Ayurvedic framework has so much to offer right now.
The Missing Clinical Trial
Despite decades of indirect evidence, no randomised controlled trial has ever directly asked: can a structured gut-healing protocol enable a deliberate, safe reduction in levothyroxine dosage?
We have abundant clinical anecdote and mechanistic plausibility, but the definitive arrow is missing.
That’s the trial that could shift guidelines.
The Gastrointestinal Blind Spot in Thyroid Guidelines
Not a single major thyroid guideline—ATA, ETA, you name it—mandates a comprehensive GI work-up for refractory hypothyroidism.
The evidence linking H. pylori, SIBO, and celiac disease to LT4 malabsorption is overwhelming, yet official recommendations remain silent.
This disconnect costs patients years of unnecessary suffering.
The Microbiome’s Black Box
A 2024 systematic review confirmed that autoimmune thyroid patients have a distinct reduction in beneficial Bifidobacterium and Lactobacillus, alongside enrichment of pro-inflammatory taxa.
But the exact metabolic cascades—SCFA profiles, bile acid transformations, TMAO pathways—that flip the autoimmune switch remain incompletely mapped.
We know the “who,” but not yet the full “how.”
The Structural Deficit
Emerging data point to decreased expression of ileal amino acid transporters LAT1 and LAT2 in some patients, directly impairing levothyroxine uptake.
This factor is almost never considered clinically, yet it represents a potential root cause entirely separate from inflammation.
These gaps aren’t just academic; they are precisely where Ayurvedic principles can guide treatment and future research.
Broader microbiome research from institutions such as Cedars-Sinai continues to reveal how bacterial overgrowth, immune dysregulation, and intestinal permeability may influence metabolic and endocrine disorders simultaneously.
Where Modern Science and Ayurveda Begin to Overlap
- Modern medicine identifies inflammation, permeability, and microbial imbalance
- Ayurveda describes the same collapse through weakened Agni and accumulated Ama
- Both systems recognize impaired transformation and blocked metabolic signalling
- Both increasingly point toward the gut as the command center
- Both agree that simply increasing medication often fails to address the root cause
Where modern science asks “what,” Ayurveda has long addressed “how to restore.”
The Ayurvedic Lens: Agni, Ama, and the Gut-Thyroid Connection
I remember the first time an Ayurvedic colleague described hypothyroidism to me not as a broken gland, but as a fire that had gone very, very quiet.
That fire is Agni—the body’s central metabolic flame.
When it burns low, a condition called Mandagni, food doesn’t transform; it half-digests and turns into a cold, sticky residue called Ama.
Think of Ama as metabolic sludge. It travels, it clogs, and it eventually finds its favourite parking spot: in a sluggish thyroid, the Srotas (micro-channels) that should carry nourishment and information become choked with it.
I couldn’t unsee the parallel to the inflammatory debris and endotoxins leaking from a damaged gut.
Same story, different language.
The Ayurvedic approach, therefore, doesn’t just “treat the thyroid.”
Instead, the emphasis shifts toward restoring digestive intelligence itself. Many of the same principles used in traditional Ayurvedic digestive restoration therapies are directly applicable to hypothyroid patients struggling with bloating, sluggish elimination, nutrient malabsorption, and inflammatory gut dysfunction.
It clears the source of Ama (the gut), re-ignites Agni, and only then rejuvenates the gland.
The Core Ayurvedic Logic
- Weak digestion leads to incomplete transformation
- Incomplete transformation creates Ama
- Ama blocks circulation and metabolic communication
- Blocked channels impair tissue nourishment and hormonal balance
- Healing requires rekindling digestion before rebuilding the system
That sequence is everything.
The Solution: A Three-Phase Integrative Ayurvedic Gut-Thyroid Healing Protocol
What follows is a structured, phased protocol I’ve refined in clinical practice, integrating evidence from Ayurvedic trials and modern gut science.
It’s adaptable but most effective under guidance.
Phase 1: Ignite & Cleanse (Weeks 1–4)
Agni Deepana & Ama Pachana
The objective is simple: reignite digestive fire and dissolve the sludge.
Without this step, any repair work you attempt will be undermined by the ongoing production of Ama.
Dietary Anchor
Shift entirely to warm, cooked, moist, easily digestible foods.
The classic Ayurvedic mono-diet of khichadi (mung beans and rice, well-spiced) is a therapeutic mainstay.
Stewed apples, ginger-spiced broths, steamed seasonal vegetables—all ideal.
Cold, raw, heavy, and mucus-forming (Kapha-aggravating) foods—dairy, wheat, fried items, processed sugars—are temporarily eliminated.
Clinically, this dietary shift alone often produces a noticeable lift in energy and a modest drop in TSH within four weeks.
Key Herbal Formulations
Trikatu (long pepper, black pepper, ginger)
The quintessential Agni deepana—it stokes the digestive fire, improves gastric emptying, and reduces post-prandial bloating.
Triphala
A gentle colon cleanser that supports downward elimination without laxative dependency, clearing the first channel of Ama accumulation.
A 2023 randomised clinical trial on an integrative Ayurveda protocol—including diet, yoga, and a polyherbal formula with Trikatu—showed highly significant TSH reduction (p<0.0001) in hypothyroid patients.
The gut-centric Phase 1 is the critical entry point.
Phase 2: Seal & Shield (Weeks 4–12)
Sroto Shodhana & Gut Barrier Repair
Only once Ama production is reduced can we effectively repair the intestinal barrier and calm the inflammatory loop that disrupts thyroid conversion.
This is where Ayurvedic medicine for thyroid and gut health truly integrates with biomedical targets.
Herbal Specifics with Modern Correlates
Curcuma longa (Turmeric)
Curcumin modulates NF-κB signalling, protects tight junction proteins (claudin-1, occludin), and reduces zonulin.
I often pair a liposomal curcumin preparation with whole-herb turmeric in cooking.
Glycyrrhiza glabra (Licorice)
Deglycyrrhizinated licorice (DGL) soothes the mucosa; whole licorice root, used judiciously, fortifies the gut barrier as a gentle demulcent.
Boswellia serrata (Indian Frankincense)
Boswellic acids are documented to preserve the intestinal epithelial barrier at physiological doses.
Kanchanara Guggulu
Although traditionally a thyroid Rasayana, this formulation’s lekhana (scraping) and lymph-clearing actions make it ideal here—it starts removing residual Ama already lodged in thyroid and lymphatic tissues.
A clinical study on suboptimal-controlled primary hypothyroidism showed that a whole-system Ayurveda protocol including Kanchanara Guggulu produced significant TSH improvement (p=0.02) compared to standard care alone.
During this phase, patients often describe a “lightening”—less bloating, clearer skin, and a first real uptick in energy and warmth.
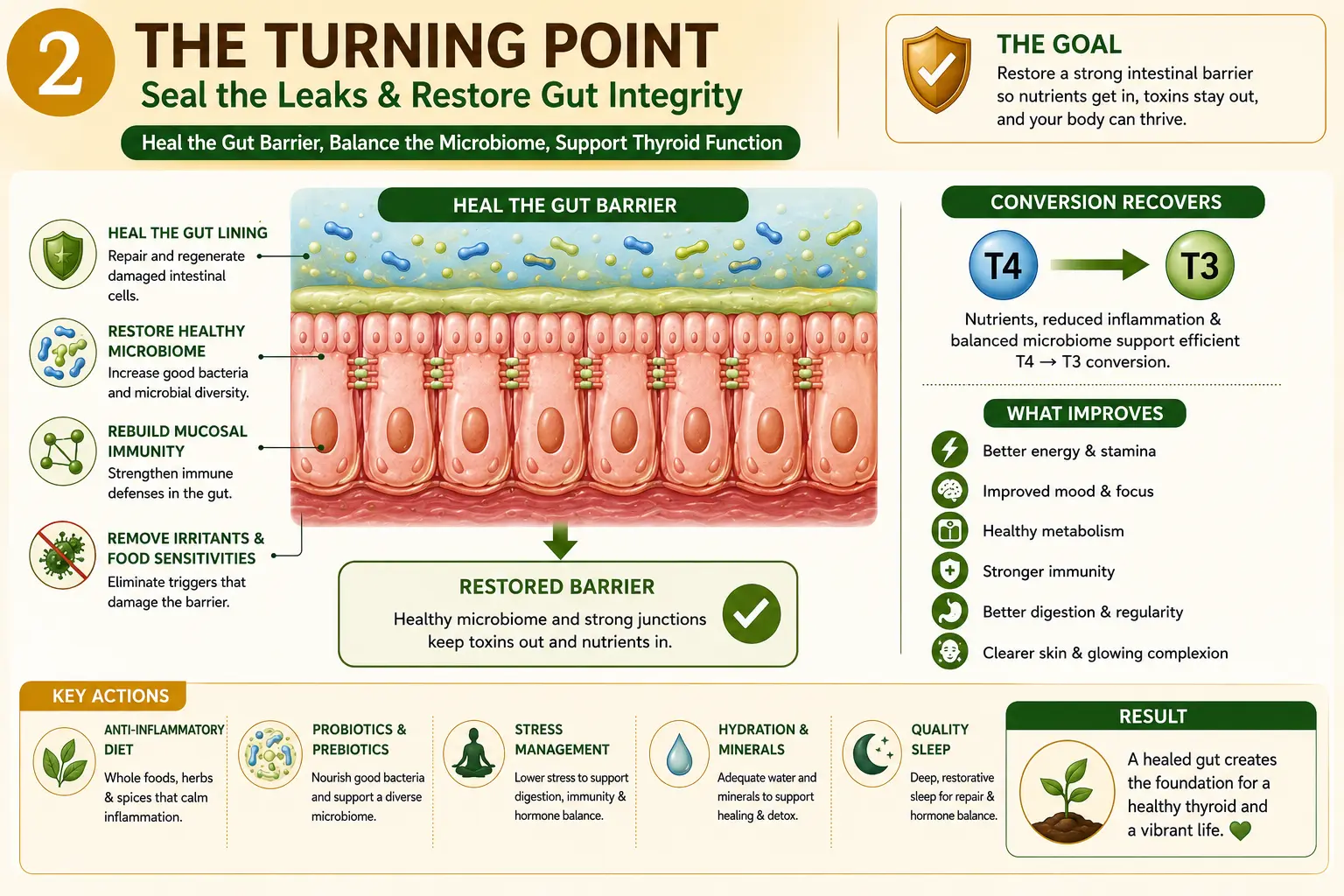
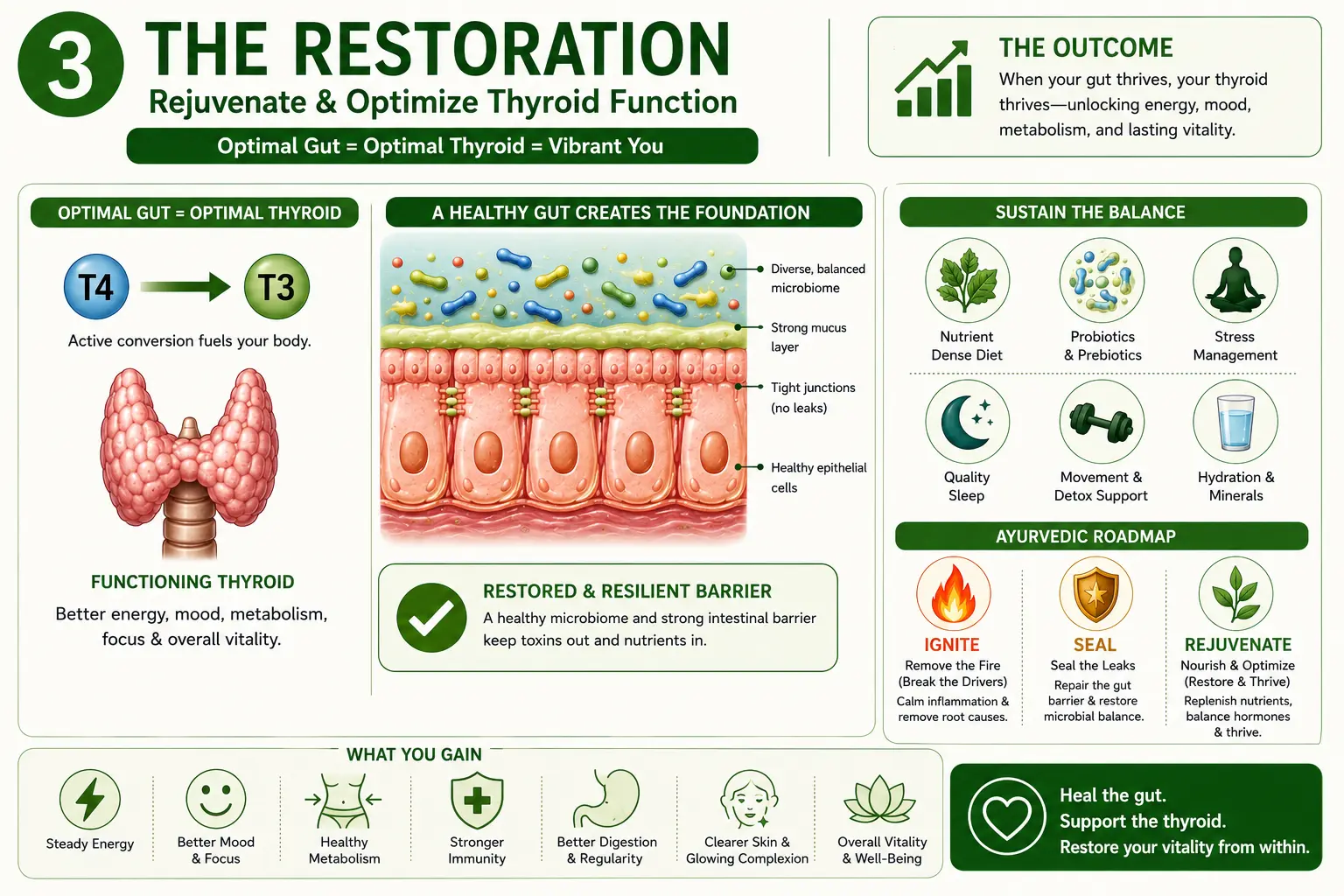
Phase 3: Rejuvenate & Restore (Month 3 Onwards)
Rasayana & Long-Term Resilience
Now we pivot from repair to deep rejuvenation.
A sealed gut absorbs levothyroxine efficiently; a rejuvenated metabolism converts it better.
This is where we deploy Ayurvedic herbs for thyroid that also sustain gut health.
Thyroid-Specific Herbal Support
Ashwagandha (Withania somnifera)
An adaptogen that moderates the HPA axis, lowers cortisol, and calms autoimmune flares.
It subtly nourishes the thyroid and supports T4-to-T3 conversion—but must be used only after Ama is cleared; giving it too early can worsen stagnation.
Other Guggulu Formulations
Triphaladya Guggulu and Punarnavadi Kashaya have demonstrated direct TSH-lowering effects in clinical studies and are chosen based on individual Dosha imbalance.
Gotu Kola & Brahmi
Often added to address the persistent brain fog that physical improvements alone don’t fully resolve.
The Gut-Thyroid Resilience Diet (Long-Term Maintenance)
We broaden the diet while keeping AIP and Sattvic principles central.
Priority nutrients include zinc (pumpkin seeds, sesame), selenium (sunflower seeds, shiitake mushrooms), magnesium (soaked almonds, cooked greens), and iron (raisins, lentils with vitamin-C-rich accompaniments).
A 2024 review confirmed these micronutrient cofactors are indispensable for deiodinase activity and hormone synthesis.
Meals stay warm and spiced; mindful eating is non-negotiable—a simple practice with profound effects on Agni.
Lifestyle Integration
Yoga & Pranayama
Sarvangasana (shoulder stand), Matsyasana (fish pose), and Ujjayi pranayama are traditionally used to stimulate the throat center.
Morning Surya Namaskar (sun salutations) rebuilds metabolic warmth.
Structural alignment and physical circulation matter more than many people realize as well. Chronic muscular tension, sedentary patterns, and postural compression can negatively influence lymphatic drainage, stress signaling, circulation, and even digestive motility. Restorative movement therapies similar to those used in structural body restoration programs can complement metabolic and gut-focused healing protocols remarkably well.
Dinacharya (Daily Routine)
Anchoring meals, sleep, and activity to the body’s circadian clock harmonizes cortisol rhythms, which directly influences thyroid hormone activation and gut motility.
This three-phase approach isn’t a quick fix.
But followed assiduously, it consistently delivers what medication adjustments alone often cannot: stable or reduced levothyroxine requirements, and a TSH that reflects genuine well-being, not just a number.
Frequently Asked Questions (FAQ)
Absolutely. An inflamed, hyperpermeable small intestine physically can’t absorb levothyroxine properly. The dysbiosis that goes hand-in-hand with leaky gut further disrupts hormone recycling and fuels systemic inflammation that blunts thyroid signalling.
Watch for: needing progressively higher doses to hold the same TSH, persistent hypothyroid symptoms (fatigue, weight gain, brain fog, cold intolerance) despite a normal TSH, and digestive clues like bloating, acid reflux, food sensitivities, or irregular bowel movements.
A levothyroxine absorption test can confirm the suspicion.
Most people notice digestive improvements (less bloating, better energy) within 2–4 weeks of Phase 1.
Meaningful shifts in thyroid medication requirements usually become apparent after 8–12 weeks, once the gut barrier is substantially repaired.
Full recalibration may take 3–6 months.
Key players: Kanchanara Guggulu (clears lymphatic congestion and supports thyroid), Trikatu (ignites digestive fire), Triphala (gentle colon detox), Ashwagandha (adaptogenic thyroid support), and Turmeric/Licorice/Boswellia (gut barrier repair).
They aren’t taken randomly—they’re used within a phased protocol for maximum safety and benefit.
Yes, when supervised.
The protocol improves absorption and conversion, which may necessitate careful monitoring and possible dose adjustment.
Never self-adjust; thyroid function should be checked every 6–8 weeks during active gut healing.
Bringing It All Together
We don’t need to wait for the perfect RCT to start using the leaky gut–thyroid axis in the clinic.
The evidence we do have—from absorption studies, zonulin data, and the quiet consistency of patients getting better on gut-first protocols—already points in one direction.
And when you layer on the ancient Ayurvedic sequence—first ignite the fire, then clear the sludge, then seal the barrier, and only then rejuvenate the gland—you’re not being “alternative.”
You’re being thorough.
You’re treating the gut like the command center it actually is.
And if that means a patient finally feels warm, clear-headed, and alive again on a stable—maybe even lower—dose of medication, then the thyroid prescription wasn’t the problem.
The gut simply needed to be ready to receive it.
Key Takeaways
- Persistent hypothyroid symptoms can exist despite “normal” TSH levels
- Leaky gut may impair levothyroxine absorption and hormone conversion
- SIBO, H. pylori, gluten sensitivity, and mycotoxins are common hidden drivers
- Ayurveda approaches hypothyroidism through restoring Agni and clearing Ama
- A phased gut-first protocol may improve thyroid responsiveness and reduce medication instability
Continue Exploring Gut & Thyroid Healing
For a deeper dive into the Ayurvedic perspective on Agni and Ama, see our companion guide, The Ayurvedic Approach to Gut Health: From Digestion to Immunity .
To explore evidence-based solutions for SIBO and thyroid dysfunction, visit our resource library.
Final Clinical Perspective
The future of thyroid care may not lie in endlessly adjusting medication doses.
It may lie in understanding why the body stopped responding in the first place.
The gut-thyroid axis is no longer a fringe theory. Between microbiome research, permeability science, autoimmune signalling, and centuries-old Ayurvedic frameworks centered around Agni and Ama, the pattern is becoming difficult to ignore.
A damaged gut changes hormone absorption.
It changes conversion.
It changes immune signalling.
And ultimately, it changes how a patient feels — regardless of what the lab report says.
That’s why the most effective long-term strategy is often not simply increasing levothyroxine, but restoring the terrain the medication depends on.
Need Personalized Gut & Thyroid Healing Support?
If you’re struggling with persistent hypothyroid symptoms despite medication, it may be time to investigate the deeper gut-thyroid connection with a more personalized functional and Ayurvedic approach.
Book A Holistic Health Consultation

